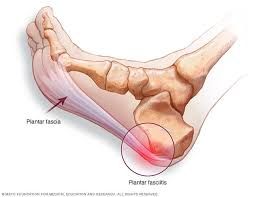
Plantar fasciitis is a common condition affecting millions of people worldwide. It's characterized by heel pain caused by inflammation of the plantar fascia, a thick band of tissue that connects the heel bone to the toes. Whether you're an athlete or spend long hours on your feet at work, understanding plantar fasciitis, its causes, prevention strategies, and treatment options is crucial for finding relief and restoring mobility.
What is Plantar Fasciitis? Plantar fasciitis typically manifests as stabbing pain near the heel, especially with the first steps in the morning or after prolonged periods of rest. The condition often develops gradually, resulting from repetitive strain or overuse, leading to small tears in the plantar fascia. Factors such as high-impact activities, improper footwear, obesity, and foot mechanics issues can exacerbate the condition.
How Does it Occur? The plantar fascia plays a vital role in supporting the arch of the foot and absorbing shock during activities like walking, running, or jumping. When subjected to excessive stress, the fascia becomes inflamed, causing pain and stiffness. Activities that place repetitive stress on the feet, sudden increases in physical activity, or inadequate footwear can trigger or exacerbate plantar fasciitis.
How to Prevent it? Preventing plantar fasciitis involves adopting lifestyle modifications and habits that reduce strain on the feet. Some preventive measures include:
- Choosing supportive footwear with adequate arch support and cushioning.
- Gradually increasing the intensity and duration of physical activities.
- Incorporating stretching exercises for the calf muscles and plantar fascia into your daily routine.
- Avoiding prolonged periods of standing or walking on hard surfaces.
How Can You Treat it?: Effective management of plantar fasciitis often requires a multifaceted approach, combining conservative treatments and therapies tailored to individual needs. Some treatment options include:
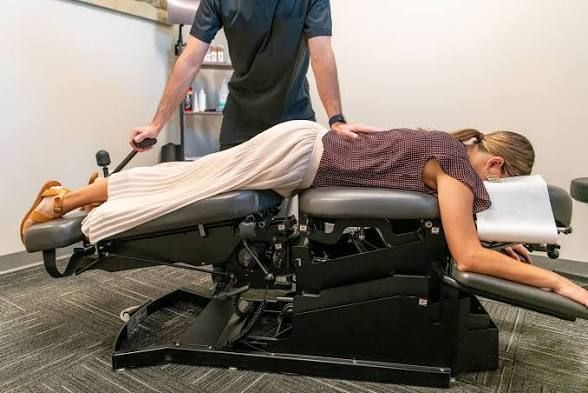
- Chiropractic Care: Chiropractic adjustments can help realign the foot and ankle joints, improving biomechanical function and reducing stress on the plantar fascia. Additionally, chiropractors may employ techniques such as soft tissue therapy to alleviate muscle tension and promote healing. They may use a technique called IASTM or Instrument Assisted Soft Tissue Mobilization otherwise known as Graston. The scraping can break up scar tissue and adhesions which can reduce inflammation and restore range of motion.
- Massage Therapy: Massage techniques targeting the feet, calves, and lower limbs can help improve circulation, reduce inflammation, and alleviate muscle tightness associated with plantar fasciitis. Deep tissue massage, myofascial release, and trigger point therapy are commonly used to address pain and stiffness.
- Orthotic Devices: Custom orthotic inserts can provide support and cushioning, redistributing pressure on the feet and reducing strain on the plantar fascia.
- Physical Therapy: A structured exercise program prescribed by a physical therapist can strengthen the muscles of the foot and ankle, improve flexibility, and enhance overall foot mechanics.
- Rest and Ice: Resting the affected foot and applying ice packs can help reduce inflammation and alleviate pain during acute flare-ups.
Plantar fasciitis can significantly impact daily activities and quality of life, but with proper care and management, relief is attainable. By understanding the causes, adopting preventive measures, and exploring treatment options such as chiropractic and massage care, individuals can take proactive steps toward healing and restoring optimal foot health. If you're experiencing persistent heel pain or suspect plantar fasciitis, don't hesitate to consult with our Buffalo chiropractors and massage therapists for personalized evaluation and treatment recommendations. Your feet deserve the best care for a pain-free and active lifestyle.
Bethany Wolcott
D’Youville Chiropractic ‘26