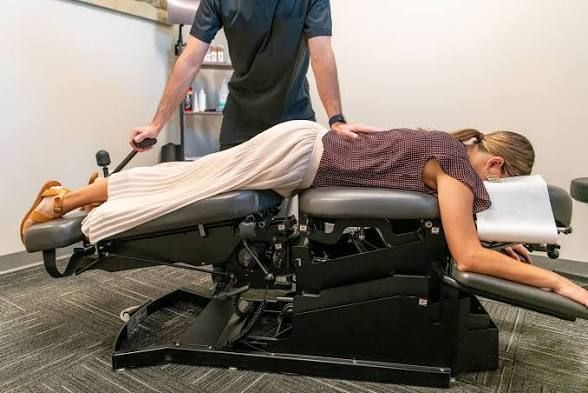
If you’ve ever heard someone say, “I don’t love the twisting and popping,” when talking about chiropractic care, flexion and distraction might be exactly what they’re looking for. This technique is one of the most comfortable, controlled, and patient-friendly tools chiropractors use—especially when dealing with sensitive or irritated spinal conditions. Let’s break down what flexion and distraction is, how it works, and when it’s typically used for both the low back and the neck. What Is Flexion & Distraction? Flexion and distraction is a specialized chiropractic technique performed using a segmented treatment table that gently moves with the patient’s body. Instead of quick thrusts or high-velocity adjustments, this approach uses slow, rhythmic motions to stretch and mobilize the spine. The name says it all: Flexion refers to bending forward. Distraction refers to a gentle pulling or decompression. Together, these movements create space within the spine while improving motion in a controlled and comfortable way. Patients often describe it as a “stretching” sensation rather than a traditional adjustment. How Does It Work? At its core, flexion and distraction works by reducing pressure in the spine and improving mobility. Here’s what’s happening behind the scenes: 1. Decompression of spinal joints and discs The gentle distraction (pulling) motion helps create space between the vertebrae. This can reduce pressure on intervertebral discs and nearby nerves—especially helpful if something is irritated or inflamed. 2. Improved disc mechanics For patients dealing with disc bulges or herniations, flexion movements can help encourage better positioning of the disc material. Think of it as giving the disc a little room to “breathe” and settle. 3. Reduced nerve irritation When spinal joints are compressed or inflamed, nerves can become irritated. By relieving pressure and improving motion, this technique can help calm things down. 4. Increased circulation and mobility The repetitive, gentle motion promotes blood flow and helps loosen stiff joints and surrounding soft tissues. One of the biggest advantages? It’s highly customizable. Chiropractors can control the speed, depth, and range of motion, making it appropriate for a wide range of patients—from those in acute pain to those simply looking to improve mobility. Flexion & Distraction for the Low Back and SI Joints This is where flexion and distraction is most commonly used—and where it really shines. The lumbar spine (low back) and sacroiliac (SI) joints take on a lot of stress from daily activities like sitting, lifting, and bending. When something goes wrong here, it can lead to stiffness, sharp pain, or even symptoms that travel into the hips or legs. Common conditions treated in this region include: Low back pain (acute or chronic) Disc bulges and herniations Sciatica Degenerative disc changes Facet joint irritation SI joint dysfunction During treatment, the patient lies face down on the table and the lower half of the table gently pulls out. The chiropractor stabilizes part of the spine and gently flexes the lower half of the table up and down while stabilizing segments of the lumbar spins. The table assists in creating smooth, controlled movement. The chiropractor may also use a side-to-side or figure 8 motion to aid in opening up the disc spaces. Why it works so well here: It reduces compression in the lumbar spine It allows targeted treatment of specific segments It avoids aggressive movements that may aggravate symptoms For patients who are flared up or hesitant about more forceful techniques, this can be a game changer. What About the SI Joints? The SI joints—where the spine meets the pelvis—are small but mighty troublemakers. When they become stiff or irritated, they can cause pain in the low back, glutes, or even mimic sciatica. Flexion and distraction can help by: Improving motion between the sacrum and pelvis Reducing stress across the joint Addressing surrounding muscle tension Because the movements are gentle and controlled, it’s particularly useful for patients with sensitive or inflamed SI joints. Flexion & Distraction for the Cervical Spine While many people associate this technique with the low back, it can also be adapted for the cervical spine. The neck is a more delicate area, so treatments here are even more precise and controlled. Instead of large movements, the chiropractor uses small, targeted motions to create decompression and improve mobility. Common conditions treated in the neck include: Neck pain and stiffness Cervical disc issues Radiating pain into the shoulders or arms Headaches related to neck tension Postural strain from desk work or device use How it helps: Gently relieves pressure on cervical discs Reduces irritation of nerves traveling into the arms Improves range of motion without aggressive force For patients who feel uneasy about traditional neck adjustments, this approach can feel much more approachable and comfortable. What Does It Feel Like? One of the most common questions patients ask is, “Is it going to hurt?” Short answer: typically, no. Most patients find flexion and distraction to be: Relaxing Gentle Rhythmic Stretch-like In fact, some people are surprised at how subtle it feels—especially compared to what they expect from chiropractic care. That said, if you’re already dealing with a painful condition, you may feel mild discomfort at first. But the goal is always to work within your tolerance and gradually improve how things feel over time. Who Is a Good Candidate? Flexion and distraction is a great option for a wide range of patients, including: People with acute low back pain Patients with disc-related issues Those with nerve-related symptoms (like sciatica) Individuals who prefer a gentler approach Patients who are sensitive to traditional adjustments It’s also commonly used for patients who are early in care and may not yet tolerate more direct techniques. When Is It Not the Best Fit? While this technique is versatile, it’s not always the first choice in every situation. Certain conditions may require different approaches or modifications. That’s why a thorough evaluation is key—so your provider can determine the safest and most effective treatment plan for you. The Bottom Line Flexion and distraction is one of the most patient-friendly techniques in chiropractic care. It’s gentle, controlled, and highly effective for reducing pressure in the spine while improving mobility. Whether it’s being used for the low back, SI joints, or even the neck, the goal is the same: restore motion, reduce irritation, and help you move more comfortably. If you’ve been dealing with back or neck discomfort—or if you’ve been hesitant to try chiropractic care because you’re unsure about traditional adjustments—this technique might be worth exploring. As always, if you have questions about whether flexion and distraction is right for you, bring it up at your next visit. Your provider can walk you through what to expect and tailor care to your comfort level and goals. Bethany Wolcott D’Youville Chiropractic ‘26
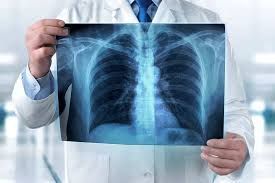
When something hurts, it’s natural to want answers—and fast. While a thorough history and physical exam are often the first step in understanding what’s going on, medical imaging can provide a deeper look inside the body. From bones to soft tissues to internal organs, different imaging tools give different kinds of information. If you’ve ever wondered what separates an X-ray from an MRI—or why one might be used over another—this guide breaks it all down in a clear, practical way. X-Ray: The Classic First Look X-rays are often the most familiar type of imaging. They’ve been around for over a century and are typically the first line when evaluating injuries, especially involving bones. How it works: X-rays use a small amount of ionizing radiation to create images of the body. Dense structures like bone absorb more radiation and appear white on the image, while softer tissues appear in shades of gray. What it’s best for: Fractures and dislocations Joint alignment Signs of arthritis (like joint space narrowing or bone spurs) Spinal structure and posture Why it’s used: X-rays are quick, widely available, and cost-effective. If someone takes a fall, has persistent joint pain, or needs a baseline look at bone structure, this is often the starting point. Limitations: X-rays don’t show soft tissues (like muscles, ligaments, or discs) very well. So while they’re excellent for bones, they won’t give the full picture for many soft tissue injuries. MRI: The Soft Tissue Specialist Magnetic Resonance Imaging (MRI) is a powerful tool when it comes to visualizing soft tissues in detail. How it works: MRI uses a strong magnetic field and radio waves—not radiation—to generate highly detailed images. It essentially maps how hydrogen atoms in the body respond to magnetic energy, which allows it to differentiate between various types of tissues. What it’s best for: Disc herniations and spinal cord issues Ligament and tendon injuries Muscle tears Brain and nerve conditions Joint injuries (like meniscus or labrum tears) Why it’s used: If symptoms suggest involvement of soft tissues—like radiating nerve pain, weakness, or instability—MRI provides a much clearer view than an X-ray. Limitations: MRIs take longer (often 30–60 minutes), can be noisy, and may feel uncomfortable for people who are claustrophobic. They’re also more expensive than X-rays. Additionally, people with certain implants or metal in their body may not be eligible for MRI. CT Scan: The Detailed Cross-Section A CT (Computed Tomography) scan is like a more advanced version of an X-ray that creates detailed cross-sectional images of the body. How it works: CT scans use multiple X-ray beams taken from different angles and combine them to create “slices” of the body. These slices can then be stacked to form a 3D image. What it’s best for: Complex fractures Internal bleeding Bone detail (especially in areas like the spine or skull) Evaluating trauma cases Detecting certain tumors or abnormalities Why it’s used: CT scans provide more detail than standard X-rays and are especially useful in emergency settings. They can quickly assess serious injuries and internal conditions. Limitations: CT scans use more radiation than standard X-rays, so they’re typically used when more detailed imaging is necessary. While they can show soft tissues better than X-rays, they still don’t match the level of detail provided by MRI for those structures. Ultrasound: Real-Time Imaging in Motion Ultrasound might be best known for its role in pregnancy, but it’s also incredibly useful for evaluating musculoskeletal and soft tissue conditions. How it works: Ultrasound uses high-frequency sound waves that bounce off tissues and create images in real time. There’s no radiation involved. What it’s best for: Tendon and ligament injuries Muscle strains Bursitis or fluid buildup Joint inflammation Guiding certain procedures Why it’s used: One of ultrasound’s biggest advantages is that it allows dynamic imaging—meaning you can see structures move in real time. For example, a provider can watch how a tendon glides during movement or identify abnormalities that only appear with motion. It’s also portable, relatively inexpensive, and safe for repeated use. Limitations: Ultrasound is highly operator-dependent, meaning the quality of the images depends on the skill of the person performing the scan. It also doesn’t penetrate bone well, so it’s not useful for evaluating deeper structures or anything hidden behind bone. Choosing the Right Tool Each type of imaging has its strengths, and no single option is “best” in every situation. Instead, they complement each other. X-rays are great for bones and initial assessments MRIs excel at showing soft tissues and nerves CT scans provide detailed, cross-sectional images—especially for complex injuries Ultrasound offers real-time imaging for muscles, tendons, and fluid The key is matching the imaging method to the clinical question. What are we trying to see? A fracture? A torn ligament? A disc pressing on a nerve? The answer to that question helps determine which tool is most appropriate. Why Imaging Isn’t Always Step One It might be tempting to think imaging should happen right away whenever there’s pain, but that’s not always the case. Many musculoskeletal issues—like minor strains, sprains, or mechanical back pain—can be effectively assessed and managed without immediate imaging. In fact, imaging can sometimes show “abnormalities” that aren’t actually causing symptoms. For example, studies have shown that many people without back pain still have disc bulges or degenerative changes on MRI. That’s why imaging is most useful when it’s guided by a clear clinical need. The Bottom Line Medical imaging is a powerful tool that helps piece together what’s happening inside the body. Whether it’s a quick X-ray to rule out a fracture or a detailed MRI to evaluate soft tissue structures, each modality provides unique and valuable information. Understanding the differences between X-ray, MRI, CT, and ultrasound can help make sense of the process and set realistic expectations. While these technologies are incredibly advanced, they work best when used thoughtfully—paired with a thorough history and physical exam to get the full picture. At the end of the day, imaging isn’t just about seeing more—it’s about seeing what matters. Bethany Wolcott D’Youville Chiropractic ‘26
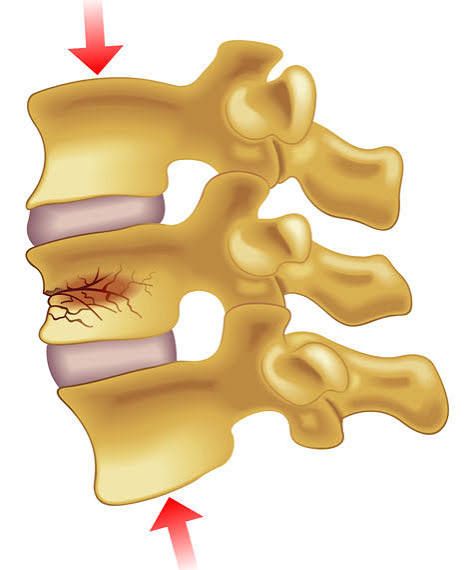
Back pain can show up in a lot of different ways — tight and achy after yardwork, sharp and stabbing after lifting something heavy, or stiff after a long day at your desk. But sometimes, back pain has a deeper structural cause. One of those causes? A compression fracture of the spine. If that sounds intimidating, take a breath. Let’s break down what a compression fracture actually is, who’s at risk, what it feels like, and how chiropractic and massage care can play a role in recovery. What Is a Compression Fracture? Your spine is made up of stacked bones called vertebrae. Think of them like a column of sturdy blocks designed to support your body, absorb shock, and protect your spinal cord. A compression fracture occurs when one of those vertebrae collapses or is compressed more than it should be. Instead of maintaining its normal rectangular shape, the front part of the bone can collapse, creating a wedge shape. These fractures most commonly occur in the thoracic spine (mid-back) and the lumbar spine (low back). What Causes a Compression Fracture? There are three primary causes: 1. Osteoporosis The most common cause of spinal compression fractures is osteoporosis — a condition where bone density decreases, making bones more fragile. As bone weakens, it doesn’t take much force to cause a fracture. Something as simple as bending forward, lifting a grocery bag, or even coughing can lead to a vertebral compression fracture in someone with significant bone loss. Postmenopausal women are particularly at risk due to hormonal changes that accelerate bone loss. Men can develop osteoporosis too, especially with aging or certain medical conditions. 2. Trauma High-impact events like car accidents, sports injuries, or significant falls can cause compression fractures — even in people with healthy bone density. 3. Pathologic Causes Less commonly, conditions such as tumors, infection, or certain cancers that spread to bone can weaken a vertebra and lead to fracture. What Does a Compression Fracture Feel Like? Symptoms can vary depending on the severity of the fracture and whether it’s acute (new) or older. Common symptoms include: Sudden onset of back pain Pain that worsens with standing or walking Pain that improves when lying down Limited spinal mobility Tenderness over a specific vertebra Gradual loss of height Increased forward curvature of the upper back (kyphosis) Some compression fractures, particularly those related to osteoporosis, can occur with minimal pain at first. Over time, multiple fractures can lead to a stooped posture and chronic discomfort. If there is numbness, weakness, or changes in bowel or bladder function, that’s a medical emergency and requires immediate evaluation. How Are Compression Fractures Diagnosed? Diagnosis typically involves: A detailed history Physical examination Imaging such as X-ray, MRI, or CT scan Imaging helps determine the age of the fracture and whether it is stable or unstable. It also helps rule out more serious causes such as infection or malignancy. If osteoporosis is suspected, a bone density scan (DEXA) may be recommended to assess overall bone health. Treatment Options Treatment depends on the cause, severity, and stability of the fracture. Conservative (Non-Surgical) Care Most stable compression fractures are treated conservatively, including: Activity modification Bracing (in some cases) Pain management Physical therapy Bone-strengthening medications (if osteoporosis is present) Healing typically takes about 8–12 weeks, though discomfort may linger longer. Surgical Options In certain cases, minimally invasive procedures such as vertebroplasty or kyphoplasty may be considered. These procedures involve injecting medical cement into the vertebra to stabilize it. Surgery is generally reserved for fractures that cause severe pain, instability, or neurological compromise. Where Does Chiropractic Care Fit In? This is an important question. Chiropractic care is not used to adjust or manipulate a fractured vertebra. If a compression fracture is acute and unstable, spinal manipulation in that area is contraindicated. However, chiropractic care can play a supportive role in recovery once the fracture is stable and healing. Here’s how: 1. Addressing Adjacent Joint Dysfunction When one vertebra is injured, the joints above and below it often compensate. This can lead to stiffness, muscle guarding, and secondary pain. Gentle, appropriate techniques may help restore motion to surrounding areas — without stressing the fracture site. 2. Postural Support Compression fractures, especially multiple ones, can contribute to increased thoracic kyphosis (forward rounding of the upper back). Chiropractors can provide guidance on posture correction and strengthening exercises to support spinal alignment. 3. Movement-Based Rehabilitation Once cleared, targeted exercises can improve core stability, spinal endurance, and balance — all critical for preventing future falls and fractures. 4. Bone Health Education Our evidence-informed chiropractic office will discuss nutrition, resistance training, vitamin D status, and lifestyle factors that impact bone density. The Role of Massage Therapy Massage therapy can be incredibly helpful — with the right approach. In the acute phase, deep tissue work directly over the fracture site is not appropriate. However, gentle soft tissue work can: Reduce muscle guarding Improve circulation Decrease compensatory tension in surrounding areas Promote relaxation (which reduces pain perception) As healing progresses, massage can help address chronic muscle tightness that develops from protective patterns and altered posture. Preventing Future Compression Fractures Prevention is key — especially for those with osteoporosis. Here are evidence-based strategies: Strength Training Weight-bearing and resistance exercises stimulate bone remodeling. Lifting weights (safely and progressively) helps maintain bone density. Balance Training Falls are a major cause of fractures. Exercises that improve balance and proprioception reduce fall risk. Nutrition Adequate protein, calcium, vitamin D, and overall nutrient intake support bone health. Avoid Smoking Smoking negatively impacts bone density and healing capacity. Routine Screening If you’re over 50, especially postmenopausal, discuss bone density screening with your primary care provider. When to Seek Evaluation You should seek medical evaluation if you experience: Sudden unexplained back pain Back pain after a fall Loss of height Increasing spinal curvature Neurological symptoms Early diagnosis makes a difference. Untreated compression fractures can lead to chronic pain, deformity, and additional fractures. The Bottom Line A compression fracture of the spine sounds dramatic — and sometimes it is. But many cases can be managed successfully with conservative care, movement-based rehabilitation, and attention to bone health. At our office, we take an evidence-informed approach to spine care. If you’ve been diagnosed with a compression fracture — or you’re experiencing new back pain and aren’t sure what’s going on — we’re here to help guide you. We’ll coordinate with your medical team when needed, modify care appropriately, and focus on helping you move safely and confidently again. If you have questions about your spine health, talk with one of our chiropractors at your next appointment. Your back supports you every day — let’s make sure you’re supporting it right back. Bethany Wolcott D’Youville Chiropractic ‘26

If you’ve ever called our office and asked, “Do you have availability for the chair?”—you’re not alone. At this point, the Back-on-Trac Decompression Chair has become something of a local legend. The name may sound intimidating (we promise, no medieval contraptions here), but the experience is quite the opposite. Comfortable, relaxing, and surprisingly gentle, this chair has earned its reputation as one of our most requested therapies. So what’s all the hype about? Let’s take a closer look at why the Back-on-Trac has become a favorite for patients dealing with back and neck pain—and why it might be exactly what your spine has been asking for. Why Spinal Compression Is Such a Big Deal Modern life is not especially spine-friendly. Long hours sitting at desks, staring down at phones, commuting, lifting kids, exercising without enough recovery, and even stress can all add up. Over time, these daily demands compress the spine, especially the discs that sit between each vertebra. These discs are meant to act like shock absorbers, but when they’re under constant pressure, they can lose hydration, bulge, or irritate nearby nerves. That’s when symptoms like stiffness, aching, sharp pain, numbness, or tingling start to show up—and they don’t always go away on their own. This is where decompression therapy comes in. Decompression Therapy: Creating Space to Heal Decompression therapy is a non-surgical, non-invasive approach designed to gently reduce pressure on the spine. Instead of forcing movement or aggressively stretching tissues, decompression works by slowly and carefully creating space between the vertebrae. The Back-on-Trac chair does exactly that. By applying a controlled, gradual stretch, it helps relieve pressure on spinal discs and nerves, encouraging improved circulation and nutrient flow to the area. When pressure is reduced, the body finally gets a chance to do what it does best—heal. A helpful way to think about it: if your spine has been feeling “compressed” by life, decompression therapy gives it room to breathe again. What It’s Like to Use the Back-on-Trac Chair One of the reasons patients love the Back-on-Trac is how comfortable and approachable it feels. You’re seated upright in a supportive chair, secured with straps to ensure proper positioning. Once the session begins, the chair applies a gentle traction force tailored to your body and condition. There’s no sudden pulling, twisting, or cracking. Most people describe the sensation as a deep, relieving stretch—often followed by a feeling of lightness or relaxation. Many patients are surprised by how calming the experience is, especially if they came in expecting something intense. Sessions are typically short, making it easy to fit into your day, and there’s no downtime afterward. You can return to work, errands, or other treatments feeling looser and more comfortable. Who Can Benefit from Back-on-Trac Decompression? Decompression therapy is especially helpful for people whose pain is rooted in disc or nerve compression. Some common conditions we see improvement with include: Herniated or Bulging Discs When discs push outward and irritate nearby nerves, pain can radiate into the arms or legs. Decompression can help reduce that pressure, easing symptoms like sharp pain, tingling, or numbness. Sciatica Pain that travels from the lower back into the hip or leg is often caused by compression of the sciatic nerve. By relieving spinal pressure, decompression therapy may help calm irritated nerves and reduce radiating pain. Degenerative Disc Changes As discs naturally lose hydration with age, the spine can become stiff and painful. Decompression helps offload stressed discs and supports healthier movement patterns. Spinal Stenosis Narrowing of the spinal canal can compress nerves and cause discomfort or weakness. Gentle decompression may help create more space and reduce symptom flare-ups. Chronic Back or Neck Tension Even without a formal diagnosis, everyday aches from posture, overuse, or stress can respond well to decompression therapy. More Than Pain Relief: The Bigger Benefits While pain relief is often the first thing people notice, decompression therapy offers benefits that go beyond symptom management. It’s drug-free. No medications, injections, or reliance on painkillers. It’s non-invasive. No surgery, no recovery period, no risks associated with invasive procedures. It supports long-term spinal health. By improving disc hydration and reducing ongoing compression, decompression therapy can help prevent recurring issues. It pairs well with chiropractic and massage care. Many patients find that decompression enhances the results of adjustments and soft-tissue work by preparing the spine to move more freely. Think of the Back-on-Trac as part of a bigger picture—one tool in a comprehensive approach to caring for your spine. Why an Initial Chiropractic Visit Matters Before hopping into the Back-on-Trac chair, we always start with an appointment with one of our chiropractors. This step is essential. Not every condition is appropriate for decompression, and we want to make sure it’s both safe and effective for you. During your initial visit, your chiropractor will review your health history, assess your spine, and determine whether decompression therapy fits into your personalized care plan. Once you’re cleared, you can schedule Back-on-Trac sessions with confidence, knowing your care is tailored to your body’s needs. We currently offer Back-on-Trac at both of our locations, making it easy to access this popular therapy. Is the Back-on-Trac Right for You? If you’ve been living with back or neck pain, feeling stiff when you wake up, or noticing that everyday activities are becoming less comfortable, decompression therapy may be worth exploring. The Back-on-Trac chair is gentle, effective, and designed to support healing—not just mask symptoms. Sometimes, the most powerful changes come from giving your body the space it needs. Ready to Try “The Chair”? The Back-on-Trac Decompression Chair has helped countless patients find relief, improve mobility, and feel more at ease in their bodies. If you’re curious about whether it’s right for you, we’d love to help. Schedule your initial chiropractic appointment today, and take the first step toward a spine that feels supported, decompressed, and ready for whatever life throws your way. Bethany Wolcott D’Youville Chiropractic ‘26
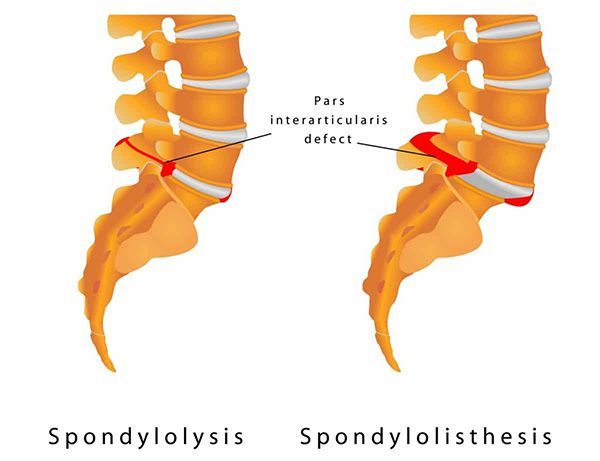
Low back pain can feel like a giant question mark. Is it a muscle strain? A disc issue? Or something with a long, hard-to-pronounce name that you heard once and promptly forgot? Two conditions that often get mixed up are spondylolysis and spondylolisthesis . They’re related, they sound almost identical, and they often involve the same area of the spine—but they are not the same thing. Understanding the difference can help you make sense of your symptoms, imaging results, and treatment options. Let’s break it down in plain English.

If you’ve ever dealt with back or neck pain, you’ve probably been told to “take pressure off the spine.” Easier said than done, right? That’s where a traction table comes in. Traction tables are a common, evidence-informed tool used in chiropractic offices to help reduce spinal compression, improve mobility, and relieve pain—without surgery or medications. Let’s break down what a traction table is, how it works, and who may benefit from incorporating traction into their care plan.
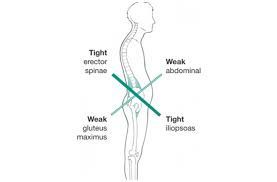
If you’ve ever stood up after a long day at your desk and thought, “Why does my lower back feel like it’s been personally offended?”—you’re not alone. In fact, your posture may be telling a whole story. Enter Lower Cross Syndrome (LCS) : a common postural pattern that shows up when certain muscle groups decide to overachieve while others go on vacation. The good news? You can absolutely fix it—and your favorite chiropractic and massage team is here to help.
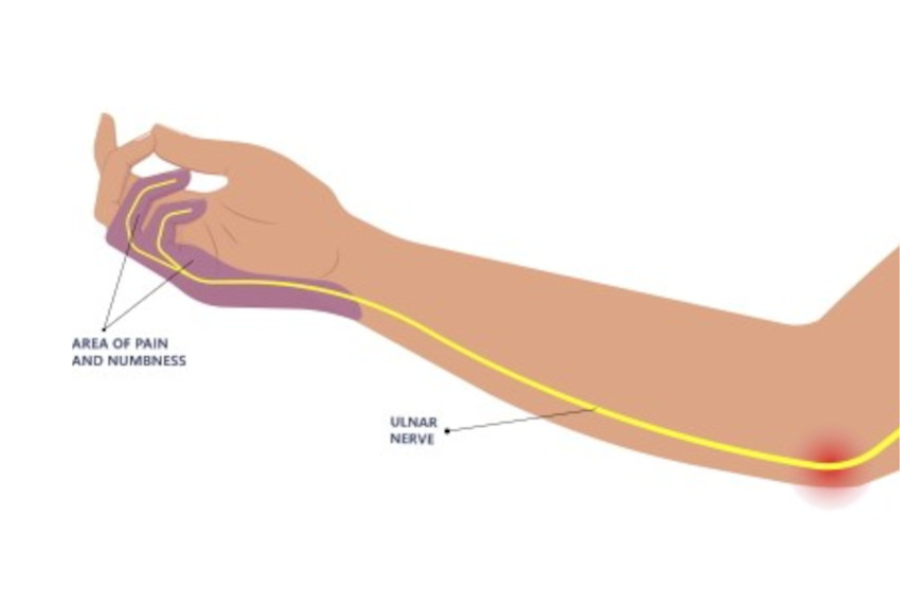
We’ve all hit our “funny bone” before — that zinger of tingling pain shooting down your arm that you shake out. But when that sensation starts happening without bumping your elbow, it might not be so funny anymore. You could be dealing with something called Cubital Tunnel Syndrome — a condition that gives your ulnar nerve a bit too much attention for comfort. Let’s break down what’s going on inside that elbow of yours, what causes this pesky problem, how to treat it, and what you can do to keep your funny bone feeling more “fun” than “numb.”