When pain starts to get in the way of everyday life, the first thing people want to know is how many visits it will take for them to feel better. When looking for the best chiropractor in Buffalo, you probably want clear answers, not vague promises.
The truth is that a lot of things affect the results. Your health history, lifestyle, and how long the problem has been there all matter. Not everyone can benefit from chiropractic care. It is a customized process that helps people move again, feel less pain, and keep their bodies working well for a long time.
Let's make it easier to understand.
How Chiropractic Care Works
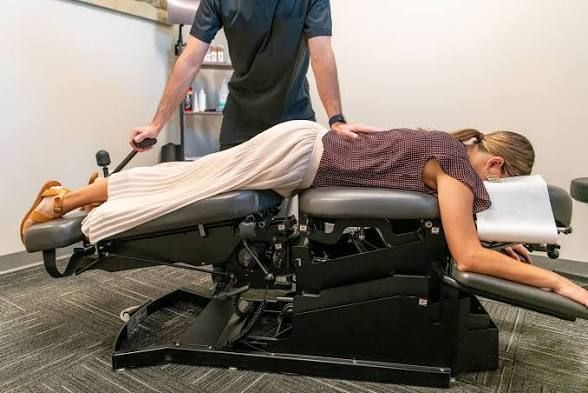
Chiropractic care looks at how the spine, joints, muscles, and nervous system all work together. When joints are out of place or too tight, they can hurt nearby nerves and make it hard to move. This can cause pain, stiffness, or swelling.
A chiropractor makes certain adjustments to get joints moving again. The body can heal faster when it can move better. A lot of patients notice changes in their pain levels, posture, and flexibility after just a few visits.
It's important to choose a chiropractor in Buffalo who looks at the whole picture, not just the symptoms, if you want the best one.
Conditions That Are Short-Term vs. Long-Term
How many times you need to see a doctor often depends on whether your condition is short-term or long-term. If you are searching for the best chiropractor in Buffalo, understanding this difference can help set realistic expectations.
Short-term conditions
Acute pain usually comes on quickly. Some examples are:
A recent strain in the back- Pain in the neck after sleeping wrong
- A small sports injury
Patients with acute cases often see improvement after three to six visits. Some people feel better after the first or second adjustment.
Long-Term Conditions
Chronic pain has been there for months or even years. This could include:
Chronic pain in the lower back- Headaches that don't go away
- Injuries from repetitive stress
Long-term conditions usually take longer. To retrain muscles and make joints more stable, the body needs care that is consistent and repeated. Depending on how bad the problem is, a care plan might call for 8 to 12 visits or more.
When looking for the best chiropractor in Buffalo, ask them how they make treatment plans for different kinds of problems.
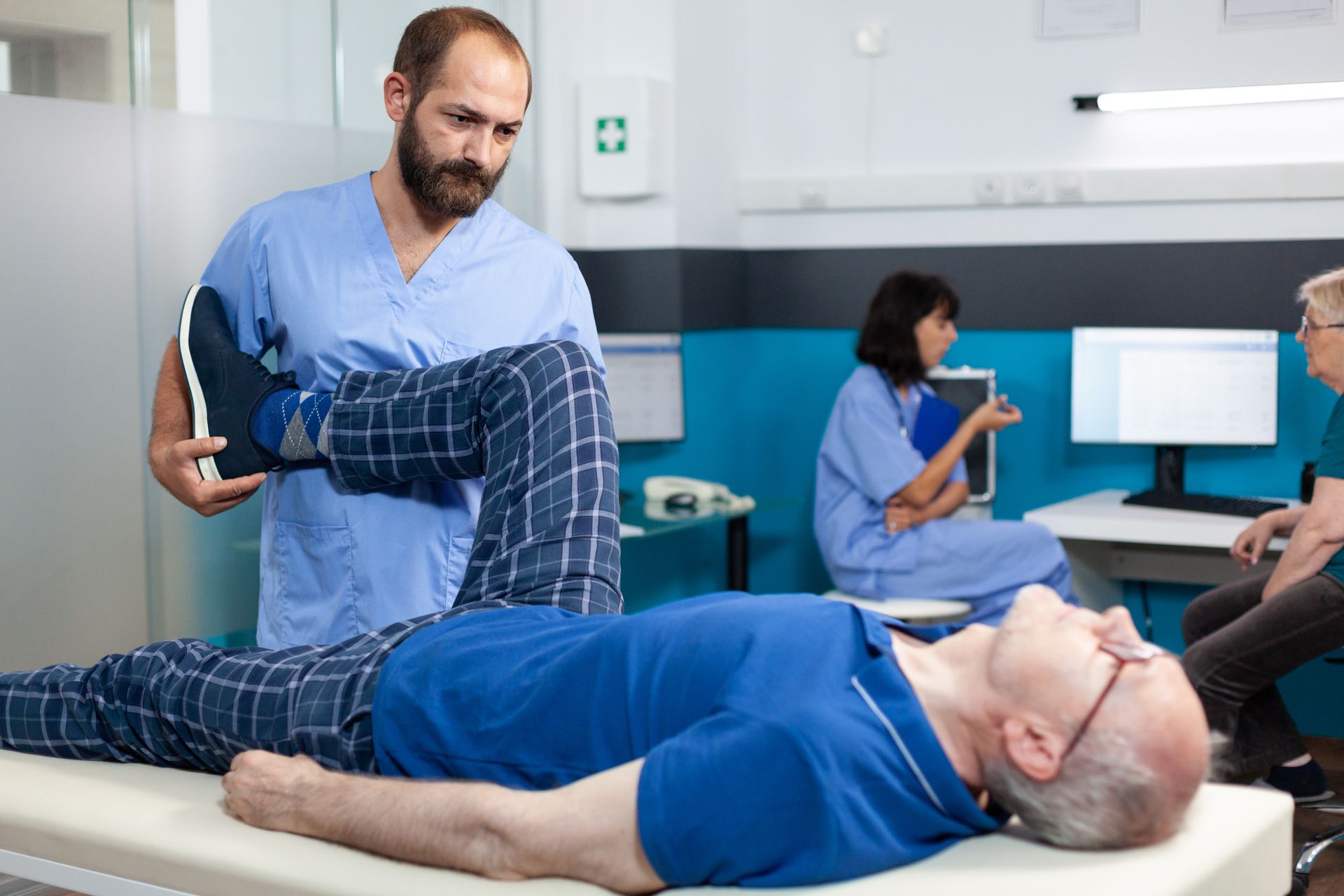
What Happens on the First Few Visits?
Usually, the first appointment includes:
A thorough medical history- Checkup of the body
- Testing the range of motion
- Assessment of posture
If it is medically necessary, imaging may be recommended in some cases. The chiropractor makes a personalized care plan based on these results.
Early visits usually focus on reducing swelling and getting the patient moving again. A lot of patients say:
Not as stiff- Better sleep
- Less severe pain
These early improvements are a good sign, but full healing may need more care.
The Common Steps in Chiropractic Care
Chiropractic care usually goes through three steps.
1. Phase of Relief
The goal is to lessen pain and swelling. You can plan visits once or twice a week. This part can last for a few weeks.
2. The Corrective Phase
Now the goal is to make joints more stable and improve muscle support. You might start doing exercises or stretches. The number of visits may go down.
3. The Maintenance Phase
Some people choose to go to the doctor every so often to keep their spine healthy and stop future flare-ups. This is up to you and your goals.
If you're looking for the best chiropractor in Buffalo, knowing these steps will help you have realistic expectations.
Things That Affect How Quickly You See Results
Each patient reacts in their own way. Several important things affect progress:
1. How bad the problem is
More serious injuries take longer to heal.
2. Length of time
The longer you've had the problem, the more sessions you might need.
3. Age and Health in General
Younger patients usually heal faster, but their overall health and lifestyle choices are also very important.
4. How active you are
Patients who follow advice on exercise and posture often get better faster.
5. Being consistent
Not going to appointments can slow down progress.
A reliable provider will make these factors clear. That openness shows that you are working with the best chiropractor in Buffalo for your needs.
What Does It Really Mean to "See Results"?
Different people may have different ideas about what results mean. For some, it means less pain. For some, it means going back to their normal daily activities, work, or sports.
In clinical practice, improvements that can be measured may include:
A wider range of motion in the joints- Less tension in the muscles
- Better posture
- Better movement that works
Pain relief is important, but to make things better for good, you also need to work on your mechanics. A chiropractor who only focuses on short-term relief may not fix the underlying problem.
When Should You Check on Your Progress Again?
A good chiropractor will keep an eye on how you respond to treatment. If there is no measurable improvement after a few visits, the way the treatment is done may need to be changed.
Some things that are red flags are:
No change in how much pain there is- Symptoms getting worse
- No improvement in function
It's important to communicate clearly and reassess. The best chiropractor in Buffalo will always put the safety and health of their patients ahead of their regular schedule.
Making Realistic Plans
Chiropractic care won't fix everything right away. It works by helping the body heal itself and improving biomechanics. That will take some time.
For a lot of patients:
Small problems get better after a few visits.- Conditions that are moderate get better in 4 to 8 weeks.
- People with chronic conditions may need corrective care for a longer time.
Instead of thinking about perfection, think about progress.
Why Personalized Care Is Important
Every spine is different. Better results come from personalized care. A full assessment can help find factors that are contributing, such as:
Bad posture- Imbalances in the muscles
- Ergonomics at work
- Too much exercise
At Peak Performance Chiropractic & Wellness, care plans are based on what the doctor finds and what the patient wants to achieve. First, we work on getting movement back, and then we work on strengthening the system to make sure it doesn't happen again.
Patients often like this personalized approach when they look for the best chiropractor in Buffalo.
What Patients Can Do
Chiropractic adjustments are strong, but the patient is just as important.
You might be asked to:
Do exercises to fix things- Fix your posture
- Change your daily habits
- Stay active and drink plenty of water.
Following these tips can speed up your recovery and make things better in the long run.
At Peak Performance Chiropractic & Wellness, we want our patients to be involved in their own recovery. Education is a part of the process, not something you think about later.
How to Tell If You've Picked the Right Chiropractor
These are the things to look for in the best chiropractor in Buffalo:
A clear explanation of your condition- Set treatment goals
- Methods based on evidence
- Regularly re-evaluating
- Talking honestly
You should feel like you know what's going on, not like you have to do something. Chiropractic care that works well is a team effort.
Final Thoughts
So, how many times do you have to go to the chiropractor before you feel better?
You might start to feel better after just a few visits for small problems. For chronic conditions, you may need to get care on a regular basis for several weeks. The exact number is different for each person.
The most important thing is to pick a provider who does a thorough evaluation, communicates clearly, and makes a plan based on your needs. A lot of people looking for the best chiropractor in Buffalo aren't just looking for pain relief. They want to see long-term progress and have a partner they can trust on their health journey.
When expectations are realistic and care is consistent, chiropractic care works best. It is possible to get meaningful results, and it is also possible to measure them.