Back pain can show up in a lot of different ways — tight and achy after yardwork, sharp and stabbing after lifting something heavy, or stiff after a long day at your desk. But sometimes, back pain has a deeper structural cause. One of those causes? A compression fracture of the spine.
If that sounds intimidating, take a breath. Let’s break down what a compression fracture actually is, who’s at risk, what it feels like, and how chiropractic and massage care can play a role in recovery.
What Is a Compression Fracture?
Your spine is made up of stacked bones called vertebrae. Think of them like a column of sturdy blocks designed to support your body, absorb shock, and protect your spinal cord.
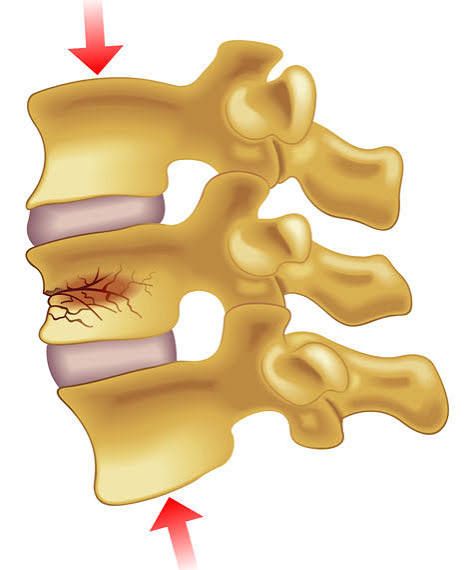
A compression fracture occurs when one of those vertebrae collapses or is compressed more than it should be. Instead of maintaining its normal rectangular shape, the front part of the bone can collapse, creating a wedge shape.
These fractures most commonly occur in the thoracic spine (mid-back) and the lumbar spine (low back).
What Causes a Compression Fracture?
There are three primary causes:
1. Osteoporosis
The most common cause of spinal compression fractures is osteoporosis — a condition where bone density decreases, making bones more fragile.
As bone weakens, it doesn’t take much force to cause a fracture. Something as simple as bending forward, lifting a grocery bag, or even coughing can lead to a vertebral compression fracture in someone with significant bone loss.
Postmenopausal women are particularly at risk due to hormonal changes that accelerate bone loss. Men can develop osteoporosis too, especially with aging or certain medical conditions.
2. Trauma
High-impact events like car accidents, sports injuries, or significant falls can cause compression fractures — even in people with healthy bone density.
3. Pathologic Causes
Less commonly, conditions such as tumors, infection, or certain cancers that spread to bone can weaken a vertebra and lead to fracture.
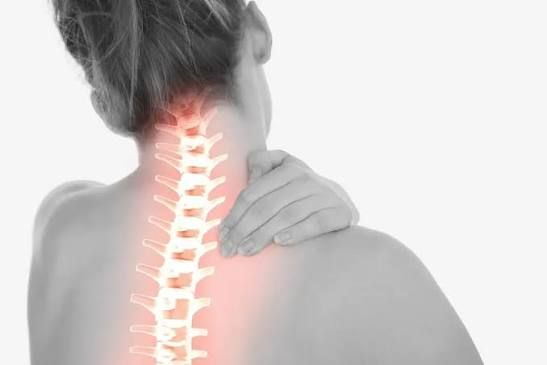
What Does a Compression Fracture Feel Like?
Symptoms can vary depending on the severity of the fracture and whether it’s acute (new) or older.
Common symptoms include:
- Sudden onset of back pain
- Pain that worsens with standing or walking
- Pain that improves when lying down
- Limited spinal mobility
- Tenderness over a specific vertebra
- Gradual loss of height
- Increased forward curvature of the upper back (kyphosis)
Some compression fractures, particularly those related to osteoporosis, can occur with minimal pain at first. Over time, multiple fractures can lead to a stooped posture and chronic discomfort.
If there is numbness, weakness, or changes in bowel or bladder function, that’s a medical emergency and requires immediate evaluation.
How Are Compression Fractures Diagnosed?
Diagnosis typically involves:
- A detailed history
- Physical examination
- Imaging such as X-ray, MRI, or CT scan
Imaging helps determine the age of the fracture and whether it is stable or unstable. It also helps rule out more serious causes such as infection or malignancy.
If osteoporosis is suspected, a bone density scan (DEXA) may be recommended to assess overall bone health.
Treatment Options
Treatment depends on the cause, severity, and stability of the fracture.
Conservative (Non-Surgical) Care
Most stable compression fractures are treated conservatively, including:
- Activity modification
- Bracing (in some cases)
- Pain management
- Physical therapy
- Bone-strengthening medications (if osteoporosis is present)
Healing typically takes about 8–12 weeks, though discomfort may linger longer.
Surgical Options
In certain cases, minimally invasive procedures such as vertebroplasty or kyphoplasty may be considered. These procedures involve injecting medical cement into the vertebra to stabilize it.
Surgery is generally reserved for fractures that cause severe pain, instability, or neurological compromise.
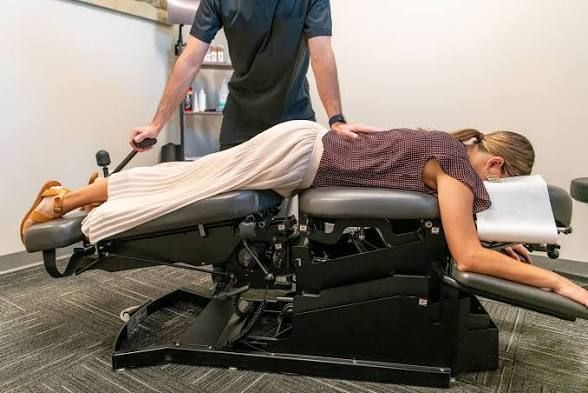
Where Does Chiropractic Care Fit In?
This is an important question.
Chiropractic care is not used to adjust or manipulate a fractured vertebra. If a compression fracture is acute and unstable, spinal manipulation in that area is contraindicated.
However, chiropractic care can play a supportive role in recovery once the fracture is stable and healing.
Here’s how:
1. Addressing Adjacent Joint Dysfunction
When one vertebra is injured, the joints above and below it often compensate. This can lead to stiffness, muscle guarding, and secondary pain. Gentle, appropriate techniques may help restore motion to surrounding areas — without stressing the fracture site.
2. Postural Support
Compression fractures, especially multiple ones, can contribute to increased thoracic kyphosis (forward rounding of the upper back). Chiropractors can provide guidance on posture correction and strengthening exercises to support spinal alignment.
3. Movement-Based Rehabilitation
Once cleared, targeted exercises can improve core stability, spinal endurance, and balance — all critical for preventing future falls and fractures.
4. Bone Health Education
Our evidence-informed chiropractic office will discuss nutrition, resistance training, vitamin D status, and lifestyle factors that impact bone density.
The Role of Massage Therapy
Massage therapy can be incredibly helpful — with the right approach.
In the acute phase, deep tissue work directly over the fracture site is not appropriate. However, gentle soft tissue work can:
- Reduce muscle guarding
- Improve circulation
- Decrease compensatory tension in surrounding areas
- Promote relaxation (which reduces pain perception)
As healing progresses, massage can help address chronic muscle tightness that develops from protective patterns and altered posture.
Preventing Future Compression Fractures
Prevention is key — especially for those with osteoporosis.
Here are evidence-based strategies:
Strength Training
Weight-bearing and resistance exercises stimulate bone remodeling. Lifting weights (safely and progressively) helps maintain bone density.
Balance Training
Falls are a major cause of fractures. Exercises that improve balance and proprioception reduce fall risk.
Nutrition
Adequate protein, calcium, vitamin D, and overall nutrient intake support bone health.
Avoid Smoking
Smoking negatively impacts bone density and healing capacity.
Routine Screening
If you’re over 50, especially postmenopausal, discuss bone density screening with your primary care provider.
When to Seek Evaluation
You should seek medical evaluation if you experience:
- Sudden unexplained back pain
- Back pain after a fall
- Loss of height
- Increasing spinal curvature
- Neurological symptoms
Early diagnosis makes a difference. Untreated compression fractures can lead to chronic pain, deformity, and additional fractures.
The Bottom Line
A compression fracture of the spine sounds dramatic — and sometimes it is. But many cases can be managed successfully with conservative care, movement-based rehabilitation, and attention to bone health.
At our office, we take an evidence-informed approach to spine care. If you’ve been diagnosed with a compression fracture — or you’re experiencing new back pain and aren’t sure what’s going on — we’re here to help guide you.
We’ll coordinate with your medical team when needed, modify care appropriately, and focus on helping you move safely and confidently again.
If you have questions about your spine health, talk with one of our chiropractors at your next appointment. Your back supports you every day — let’s make sure you’re supporting it right back.
Bethany Wolcott
D’Youville Chiropractic ‘26